Thank you for your supportive comments last week. You all delight and amaze me--you're greatly appreciated.
Within the past two weeks I received an email inquiry about the palatal expander and therapy. Also, an attendee at my seminar in Sacramento asked a specific palatal expander question. Both were good questions and motivated me to write about the topic. Thanks, you guys!
Greetings to You, Dedicated SLP!
Has a child ever walked into your therapy room and he sounded 10 times worse than he did last week? Chances are he's been fitted with a palatal expander.
We have a remediation responsibility to the child, so, now what?
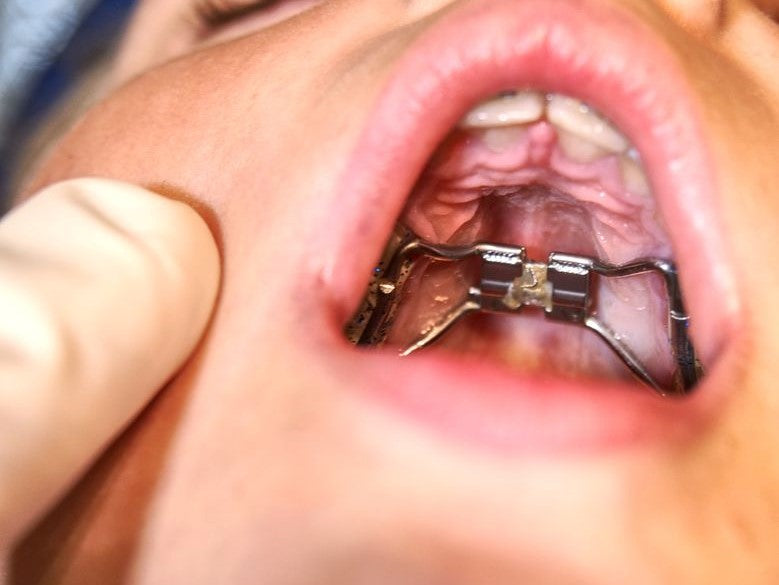
Sometimes the answer is obvious. The child's tongue in the above pic can in no way successfully learn to interact appropriately with his upper side teeth and the roof of his mouth. (Also, look at his alveolar rugae, it's super bumpy, indicating his tongue has probably NOT been resting consistently on the ridge. If it had the rugae would be less bumpy or even smooth.)
But sometimes the answer isn't as obvious and stops us in our tracks. We’ll cover some of those primary issues, and hopefully the information will add clarity to a potential conundrum.
But first, here’s a quick answer to “Does a Palatal Expander Interrupt Speech Therapy?” In a word, yes, in most cases. There are a few variables to determining the therapy-answer. Briefly, here are some things to do:
-
Analyze the invasiveness of the device. Some palatal expanders are more intrusive and lingual-limiting than others.
-
Determine if appropriate speech stabilization and mobilization--especially of the sounds you're working--can potentially be achieved, or not.
-
And, determine if is it possible for the child to come close to a good tongue-palate resting position. Why? The tongue’s resting posture determines its speech operating zone. Keep in mind, most (not all) palatal expanders encourage a lowered tongue operating zone.

Expansion Devices (Dental Arch and Palatal Arch)
An expander is an appliance fitted by an orthodontist designed to widen the upper dental arch (for dental movement), or, to widen the upper dental arch (for dental movement) AND widen the palatal arch (for skeletal/palatal growth and width).
Keep in mind the dental arch is the horizontal arch that houses the teeth; you have two of them, top and bottom. The palatal arch is the vertical arch on top; we also refer to it as the hard palate. Different, but related.
Basically, there are two types of expanders. However, there are a variety of comparable styles within each type. Most expanders are fixed and not removable and are fixed to the teeth in some way. Other expanders are removable (they’re less common).
We’ll cover the basic two types: The Rapid Palatal Expander and the Quad-Helix. These devices are typically used before braces, but not everyone who needs braces has to wear an expander first.
The Rapid Palatal Expander:In the literature, this device is frequently referred to as a Rapid Maxillary Expander (RME) (see above photo). The pressure for bony palatal expansion is activated by the periodic turning of a “screw” on the device via a special key provided to the parent/caregiver. Gradual outward pressure is placed on the left and right haves of the upper jaw. This pressure causes an increased amount of bone to grow between the halves of the jaw which results in increased width.
In addition, narrow or deep jaws can make it difficult to breath through the nose. Once the palatal arch is widened, it is not unusual for nasal breathing to improve.
The Quad-Helix: This device is used primarily for dental arch expansion. Bands are anchored to the back molars to keep it in place while four helix springs widen the arch (see above photo). This appliance is ideal for dental crowding in the upper arch or to correct a posterior crossbite. It’s a modification of the “W” appliance and sometimes the quad-Helix is referred to the “W” appliance.
The dental arch expansion helps to make room for teeth. Deciduous (baby) teeth are smaller than the adult permanent teeth. For some, the baby teeth may not appear crowed when housed in small dental arches, but when the larger permanent teeth come in, the result may be a jumble of overlapping teeth.
Here’s where the invasive variability into the palatal area comes in. Sometimes the “wires” around the perimeter of the palate touch the perimeter or even the sides of the teeth. This perimeter contact plus the relative width of the dental arch may allow the tongue to operate up within the dental arch. However, sometimes, like the one in the photo, the “wires” take up space within the palatal vault leaving limited or no room for the tongue to elevate and interact.
The Age of Insertion
Palatal expanders can be inserted as young as six (unusual) up until the time the hard palate finishes fusing, around 15 or 16 years of age. Some orthodontists recommend insertion only when all of the permanent teeth have broken through. Others feel that an expander should be used as soon as a crossbite has been detected which is frequently before the permanent teeth come in. Each orthodontist has his/her own philosophy about this.
Length of Wearing-Time
The average length of expander wearing-time is 6 to 8 months. Typically, the dental arch/palatal arch is expanded within the first weeks or months, then the device is fixed in place for the remainder of the time. This extra time insures and makes the width change permanent and prevents the arch from relapsing.
The Expander, the Child, and Speech
The presence of most palatal expanders within the mouth of a child with normal speech production will alter the way the child speaks and sounds. Some kids compensate easily, others have difficulty adapting to the presence of a palatal device and adjusting their tongue placements and movements around it.
The child with delayed or disordered speech development may have an even tougher time modifying his/her tongue movements and acclimating to the presence of the device. The appliance is fitted up within the dental arch where most of the consonants and half the vowels are produced. The risk is that his/her speech will deteriorate. It’s up to the capability of the child, the invasiveness of the device, and how abnormally narrow his/her dental arch/palate was prior to the insertion.
Does it hurt? I’m told the pain-level varies from person to person. Generally, there mild to moderate discomfort or pressure during the first few days, and again, when the key is turned. Also, there may be tongue irritation from rubbing against the metal appliance, in addition to headaches, extra saliva, and difficulty keeping the device clean. When the palate is “split” there frequently appears a space between the front central teeth (a diastema) that wasn’t there before. The presence of this space is normal and closes when the braces are put on at a later date.
Questions to ask or observations to make:
-
Does the dental arch and/or palatal arch look narrow to you?
-
Have you noticed that it’s difficult for the child to elevate his/her tongue and generate lingual-palatal contact and interaction due to space availability?
-
Does the child appear to have a narrow face? Is this due to heredity, as far as you know, or not? In other words, does someone in the family have a narrow face?
-
If there is a difference in the upper dental and/or palatal arch, what is it due to? If not heredity, is it due to excessive, chronic thumb/finger sucking? Excessive pacifier use? (Research says this one is most often the culprit.) Tongue sucking? Extreme lack of frequency of tongue-palate contact? This last one can be related to chronic mouth breathing (respiratory issues).
-
Ask the child bite his teeth together (make sure he/she does not jut the jaw forward) and look at the relationship of the top and bottom side teeth. Is there a dental crossbite? In other words, are the top side teeth (either left, or right, or both) significantly inside of the bottom side teeth? Keep in mind, it is normal for the top dental arch to be slightly wider than the bottom dental arch. This is to keep us from biting our cheeks when we chew.
In my opinion, the problem for most of us is our inherent obligation we feel toward remediating the child’s speech. There’s also the legal document, usually the IEP, that obligates us as school SLPs to see and help the child. The palatal expander throws a kink in the remediation process.
In most cases, I would recommend stopping speech therapy during the time the expander is inserted. Trying to “get speech sound” when there’s no room to do so, is not fair to the child. On the other hand, we can address anything that does not require lingual lateral margin stabilization and interaction with the alveolar ridge and hard palate. Here are a couple associated issues: Is there a habit we can address while the appliance is inserted? Can we work on extinguishing thumb/finger sucking? Can we work toward lip closure and nasal breathing?
In most cases, I am pro palate expansion. When the device has done its job and removed, the result is a more roomy, more spacious upper area for the tongue to move and interact. Typically, that’s a good thing.
Although the timeline is measured in months, and it represents almost an entire school year, the presence of the device is temporary and therapy can be continued after the device is removed.
My therapy focus is on the ease and access of lingual stabilization and mobilization for speech sounds and the tongue’s resting position. In most cases, once the tongue acclimates to its new wider environment, the outlook may be more positive for maintaining consistency of good resting postures and achieving good speech production.
Go get em! See ya next week.
All the best to you and your speech-kids,
Char Boshart
Resources:
Agarwal, A. and Mathur, R., 2010. Maxillary expansion. Int J Clin Pediatr Dent, Sep-Dec; 3(3); 139-146.
Stevens, K., Bressmann, T., Gong, SG., Tompson, BD, 2011. Impact of a rapid palatal expander on speech articulation. Am J Orthod Dentofacial Orthop; Aug; 140(2); 67-75.
Leave a comment (all fields required)
Comments will be approved before showing up.

![#71 Telepractice Tips 'n Info (Part 4) [Is my child working or just playing games?]](http://speechdynamics.com/cdn/shop/articles/Game_Pieces_and_Hand_7_x_3_2048x.jpg?v=1605804364)
